Periodontics quiz
Advanced
Quiz 5
Classification of Periodontal and peri-implant diseases and conditions (Advanced)
Results
CONGRATULATIONS!!!
Don`t give up, try again!
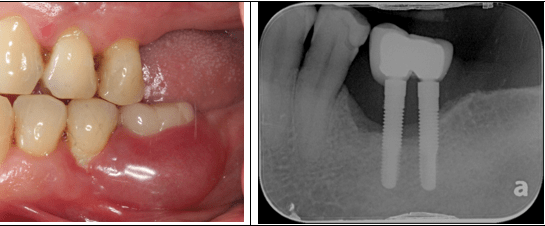
#1. What would be precise periodontal diagnosis for this patient? – For more information HOVER on the question mark !!! ? A 56 old patient presents with gum recessions and tooth mobility. Periodontal chart shows PD of 5 mm on majority of dentition. Gingival recession on affected teeth is 2mm. The following teeth have been extracted due to periodontitis: 18, 17, 16, 26, 27, 36, 35. Panoramic radiograph shows vertical bone loss on 13, 24, 25 and 35 and furcation involvement of grade II on lower second molars. Mobility of grade I is present on 31, 41 and 42. Patient is currently smoking 20 cigarettes a day.
#2. Which of the following conditions results in early presentation of advanced periodontitis and may affect both primary and secondary dentition?
#3. Which of the following diseases may affect gingiva?
#4. Main symptoms of necrotising gingivitis include.
#5. According to the Classification of the Periodontal and Peri-implant Diseases and Conditions from 2017, under which category of periodontal diseases you would classify HEREDITARY GINGIVAL FIBROMATOSIS?
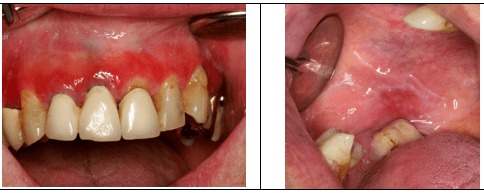
#6. A 63 years old female presents with distinctive gum redness and sensitivity. Intraoral exam indicates the presence of bilateral symmetrical lace-like lesions on inflamed buccal mucosa. Panoramic radiogram does not show any significant crestal bone loss. Which of the following conditions may have caused desquamative gingival lesions in this case?